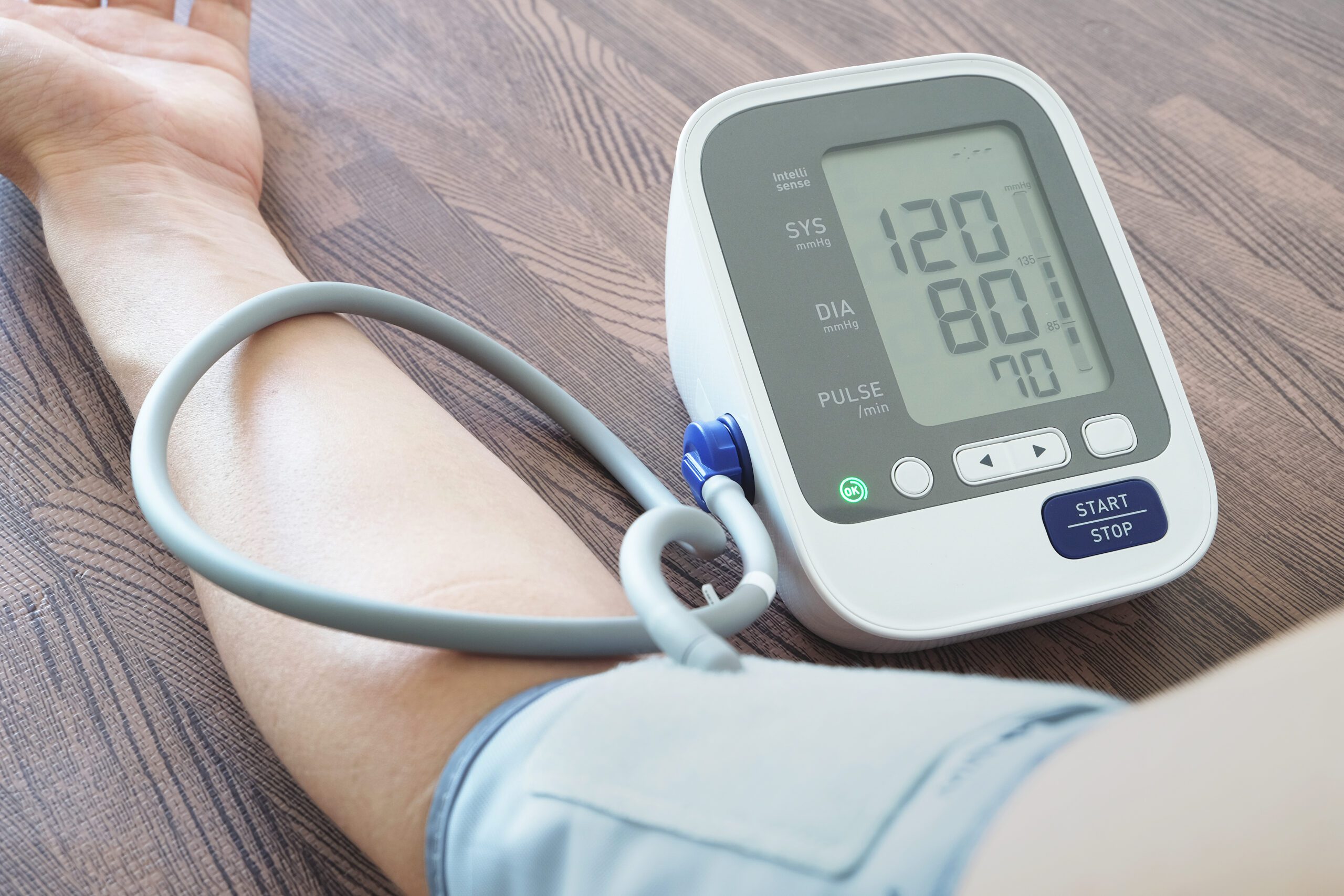
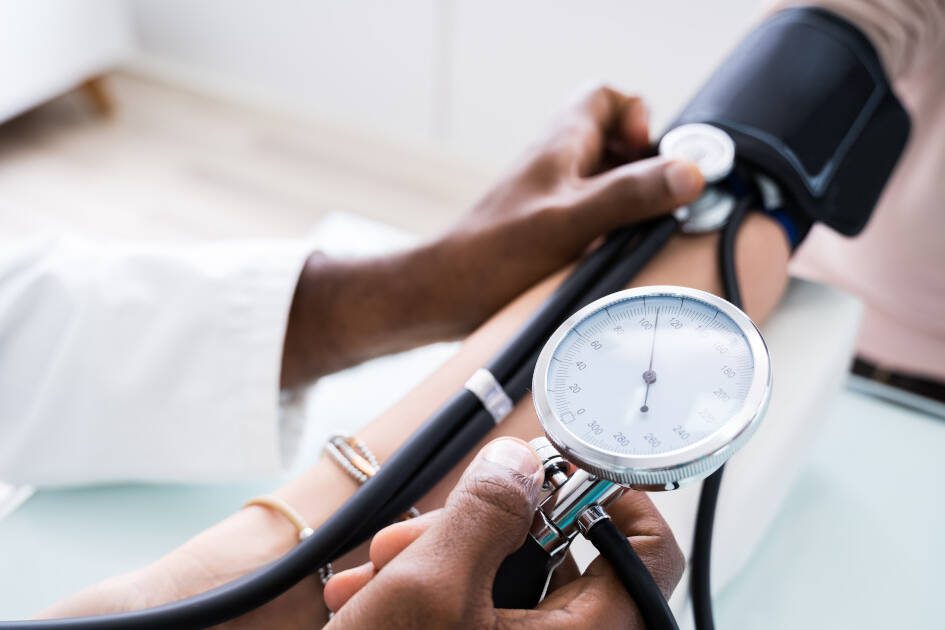
How chronic, long-term anxiety may be contributing to your high blood pressure.
Anxiety and Blood Pressure | Managing Blood Pressure | Stress and Anxiety | Lifestyle Intervention
Anxiety is one of the most common mental health issues in North America, affecting around 20% of adults1. It causes significant impacts on health and quality of life and is linked with multiple other health conditions1. Anxiety often presents as “overthinking” or “over-worrying” and can impede relationships, work and simple day to day activities. It has a reciprocal relationship with health conditions, meaning the physical symptoms may cause or worsen anxiety or the anxiety may worsen the physical symptoms. We know that treating underlying mental health conditions is an essential part of the healing process.
Hypertension, or high blood pressure, affects a similar number of people as anxiety (around 25% of adults) and is the leading cause of preventable death and disability in Canada. Hypertension is multifactorial in its cause, from genetics (or a family history of cardiovascular disease) to lifestyle choices and even psychosocial factors like stress and anxiety. We know that when we make changes to modifiable risk factors like lack of exercise, high salt intake and chronic stress, this decreases your risk of serious cardiovascular events like heart attack and stroke.
Researchers have been interested in the correlation between hypertension and anxiety for decades and the rising prevalence of both makes this relationship all the more compelling. Is anxiety associated with hypertension? Let’s find out.
White Coat Syndrome
There’s a common phenomenon termed “white coat syndrome” where acute or situational anxiety increases your blood pressure, typically in the doctor’s office2. This causes higher than normal blood pressure readings and is why we now use a 3 reading average rather than a single reading to diagnose hypertension. It also highlights the importance of at home blood pressure measurements to collect data you can share with your health care team. Check out this blog to ensure your at-home readings are accurate and reliable.
White coat syndrome helps us to understand how acute stress (which is a normal response) causes an increase in blood pressure2. However, this rise in blood pressure is temporary and isolated events of anxiety or stress like this do not cause hypertension2.
Chronic Anxiety or GAD
Acute stress is in contrast to ongoing anxiety that is not due to an isolated life event or stressful situation. Generalized Anxiety Disorder (GAD) is defined as “feeling nervous, anxious or on edge” plus “not being able to stop or control worrying” more days than not each week3. This kind of anxiety causes a baseline increase in our sympathetic nervous system (think “fight or flight”) which causes changes in our body predisposing us to having higher blood pressure1. The full mechanism connecting anxiety to hypertension is complex, but the simple part is that there is a correlation between ongoing anxiety and hypertension1.
Other Contributing Factors
While there are physiological mechanisms linking anxiety and high blood pressure, there are psychosocial factors that also contribute to this correlation. The first is, people with anxiety are more likely to engage in unhealthy lifestyle habits1. This includes things like smoking, drinking, increased eating and decreased exercise1. We know that these are modifiable risk factors for hypertension and likely contribute to the increased risk of high blood pressure.
Secondly, anxiety is a barrier to both diagnosis and treatment of hypertension4. Stress, anxiety, and depression are the most commonly reported reasons for hindering or delaying lifestyle modification, which is first line treatment for high blood pressure4. This highlights the importance of not only physical but also psychological support in hypertensive patients with anxiety.
So what can you do?
1. Don’t stress about your numbers! Feeling anxious about your daily blood pressure reading will do more harm than good. Check out this blog for ideas on how to make measuring your blood pressure a healthy habit.
2. Treat your anxiety. Talk to your healthcare provider about your options! It’s thought that a combination approach of anti-hypertensive treatment & anti-anxiety treatment (typically a combination of medication and counseling) is more efficacious than either alone.
3. Introduce mindfulness. Start to make mindfulness and stress reduction part of your everyday life. It’s a simple practice that has a scientifically proven impact on blood pressure and heart health.
Subscribe & Save
Two tablets. Every day. A lifetime of health.
Consistency is the key to maintaining healthy blood pressure levels and supporting your heart health. By taking two PreCardix® tablets every day, you’re building a daily routine that promotes long-term cardiovascular wellness and vitality.
Choose Support
Your local pharmacy is a great resource for blood pressure management. They have free blood pressure kiosks available to monitor your numbers and knowledgeable pharmacists ready to answer your questions and provide support for healthy blood pressure!
Regular blood pressure monitoring is a healthy habit and will keep you on track to reach your overall wellness goals.
References
- Pan Y, Cai W, Cheng Q, Dong W, An T, Yan J. Association between anxiety and hypertension: a systematic review and meta-analysis of epidemiological studies. Neuropsychiatr Dis Treat. 2015;11:1121-1130. Published 2015 Apr 22. doi:10.2147/NDT.S77710
- Spruill TM, Pickering TG, Schwartz JE, Mostofsky E, Ogedegbe G, Clemow L, Gerin W. The impact of perceived hypertension status on anxiety and the white coat effect. Ann Behav Med. 2007 Aug;34(1):1-9. doi: 10.1007/BF02879915. PMID: 17688391.
- Spitzer RL, Kroenke K, Williams JBW, Löwe B. A Brief Measure for Assessing Generalized Anxiety Disorder: The GAD-7. Arch Intern Med. 2006;166(10):1092–1097. doi:10.1001/archinte.166.10.1092
- Khatib R, Schwalm JD, Yusuf S, et al. Patient and healthcare provider barriers to hypertension awareness, treatment and follow up: a systematic review and meta-analysis of qualitative and quantitative studies. PLoS One. 2014;9(1):e84238. Published 2014 Jan 15. doi:10.1371/journal.pone.0084238
Important Information
Always consult with your healthcare provider before making changes to your blood pressure management plan. PreCardix® does not treat, cure, or prevent medical conditions. Measure and monitor blood pressure regularly. Know the signs of heart attack and stroke.
Do not take PreCardix® if you are under age 18, if you are pregnant or breastfeeding, have renal artery stenosis, have a history of angioneurotic edema, or have a shellfish allergy. Consult product guidelines for additional information. Print and share the product monograph with your healthcare provider.
PreCardix® is an innovation of Marealis Inc. a Norwegian Bio-Tech company dedicated to finding natural, sustainable, and effective marine-based solutions for blood pressure health, globally. Designed in Norway. Manufactured in Canada.
Prioritize Your Heart: Essential Steps for Maintaining Optimal Cardiovascular Health

Hypertension: Your Proactive Guide to Understanding and Managing High Blood Pressure